A Journey Through Postpartum Depression
Celia’s story is important; as the winner of my 2019 ‘The Story’ giveaway, I am grateful she is willing to be vulnerable and transparent in telling her journey through postpartum depression.
Postpartum depression is prevalent worldwide. In the United States, the CDC reports 1 out of 10 women reports having symptoms in the past year. Rates vary from state to state and worldwide, but some estimates are as high as 1 out of 5 women. While a history of depression and anxiety can increase the risk of postpartum depression and anxiety in women, other risk factors can play an important role, such as; poor social support, birth trauma, and recent stressful life events.
Postpartum depression has been taboo for many years, often because women and their families are afraid of speaking up about it out of shame or fear of being judged.
Celia had such a beautiful way of expressing her feelings and journey in her own words, so without any further ado, here is her story and her film.
Postpartum depression is a devastating condition that isn’t talked about enough compared to the number of women who suffer from it. These women must know they are not alone. I continuously struggle with the haunting memories and voices in my head telling me I’m a bad mother and that my son deserves more. At the same time, I feel ashamed to open up to the world regarding my condition and what feels like permanently branding me as a bad mother; that feeling pushes me to talk about it. We do NOT deserve to feel embarrassed or stripped of our character; we did not choose this. Being a mother, in my opinion, is the most selfless act. We change our bodies for ten months and carry the scars and often insecurities. We tear our bodies in labor and have next to no recovery time. For many mothers, this transition is traumatic. It’s hard to identify who you once were when there’s next to no time for yourself or doing the things that once made you feel like you.


My husband and I were thrilled when we found out we were expecting. In my heart, I always knew he was a boy. Within 13 weeks, we chose the name Oliver. I was extremely sick throughout my pregnancy; I remember being unable to eat for multiple days at a time. I was often bedridden with severe vertigo and unable to attend work.
Nonetheless, I loved every moment I got to share with my son. I read many articles on parenting, attended labor and delivery classes at our hospital of choice, prepared my hospital bag, and bought the highest-reviewed products to welcome Oliver home. Never in a million years would I have thought to prepare for what would happen.
I still get choked up thinking about the terrifying day on November 6th, 2018. I had an appointment with my high-risk pregnancy doctor, Doctor Woods, to monitor my son’s well-being. The technician searched for my son in the ultrasound, then immediately called the doctor. I was informed that I had 2 cm of amniotic fluid, and 5 cm was typically cause for concern which she would send someone to the hospital for an IV. They immediately contacted my delivery doctor. I was told I needed to deliver directly before my son went into distress and didn’t even have enough time to run home to grab my delivery bag.
Everything I had prepared for went out the window.
I expected to be sent to multiple waiting rooms (as rehearsed in my classes) but was quickly taken into a private room with multiple monitors on my stomach. The induction began almost immediately. I recall the pain being unbearable. There were no breaks in between my contractions; there was no tranquility or magic at the moment. I continued to vomit throughout the induction and recall being weak from a lack of rest, water, and food. While I most feared the epidural, I was weak and hardly conscious of its application.
Twenty-five hours later, it was finally time to push. My epidural was turned off so I would have the urge to push, but the pain was unbearable. I couldn’t tell the constant pain from contractions. I recall the nurse yelling that I had to push my son out, but I mentally shut down. My doctor was assisting another patient (later communicated to me), and the only ones in the room were my husband, a nurse, and an EMT student brought to learn. I remember crying, trying to communicate that I couldn’t push him through, no matter how hard I tried. Instead, my nurse took the route of “tough love” and told me, “well, it’s too late” or “you have to.”
I felt backed into the corner, in pain, with no-one understanding that my son would not fit (perhaps through the stress and fear I was physically not stretching). In what felt like an eternity later, my doctor appeared, and I received an episiotomy. My son was delivered on November 7th, but it was not a magical moment.

I lay there, shaking from the pain, while the medical supplies on my doctor’s gown (probably a stethoscope) reflected the bloody mess of my flesh being sewn…slowly. It was like a nightmare, I recall pleading for something to help with the pain, but no one listened.
I felt embarrassed. All the courage I had practiced, the selflessness of reminding myself, “all that matters is getting my son here safely,” had failed me. I was simply the worst patient of their day, the mother who couldn’t do what all women’s bodies were built to do. There was no time to focus on my mental health; immediately, I was told it was time for “skin-to-skin contact” and nursing. My son immediately loved me. When they handed him to me, he knew I was his mother and stopped crying. When my family tried to hold him, he cried until he was in my arms once more. I, however, did not feel that bond. Instead, I felt duty. I knew my duty was to nurse him every two hours, to do everything the doctors instructed me to do.
Reflecting on it now, after all the traumatic months my body endured, it was vital for me to rest. Instead, I bore additional responsibilities with no rest. I was too busy adjusting to my new list of duties to slow down and ask myself if I was ok if I needed help.


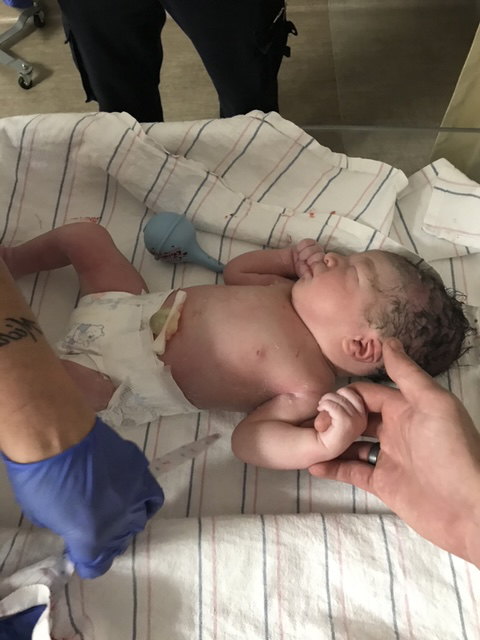

I was discharged on November 8th. I recall the night it “hit me.” My husband asked to shower, and for the first time, I would be left alone with my son, who was resisting rest. As I sat there, an overwhelming flood of emotions hit me. I did not want this life; I had made a huge mistake. I was not fit to be a mother, and there was no going back. What would everyone think of me? What would my husband say? Would he leave me? I broke down crying and could not stop. I was in the darkest place. My life felt like a box of emptiness, and everywhere I turned was a wall telling me I could not get out.

I remember watching my husband confronted with the news, the exhausted look on his face as he desperately tried to put my son to sleep. He looked miserable. But I could not get up—the weight of these emotions lay over my body. I couldn’t move. I insulted myself and ensured I felt every bit of the self-deserving misery for being selfish and ordered myself to get up…but I could not”
Although my family told me to call them if I needed anything, I was too ashamed. I asked my husband if we could call his mother because she had previously offered to stay the night if we needed her. I fell asleep during the time that she arrived. Whispers awoke me outside of my bedroom. She told him it was too late for me to change my mind, that it was motherhood and I needed to get up. Dread filled me; could anyone help? Was I stuck?

Suddenly I no longer felt like an adult; I felt like a pathetic child being scolded. Early in the morning, she awoke me to breastfeed my son. I struggled as he failed to latch and screamed of hunger. His cries pierced through me; I hated being a mom. I hated breastfeeding. But I couldn’t tell her that because I feared judgment.
While our son slept, we called every hotline we could google. We even called the hospital and my OBGYN office. The hospital staff asked to speak with me and asked if I would hurt my child or myself. I was terrified they’d take my child and felt disgusted at myself for even being a risk. When they felt I wasn’t an immediate threat, they told me they suggested getting admitted to a psychiatric ward. I asked what would become of my son and husband, who was also a first-time father and was told they’d be fine without me.

We went to my sister’s house to visit my family. The truth is it brought comfort being surrounded by parents who know how to attend to my son. They held him while I lay. Still, I stayed silent about my feelings and what I was experiencing, hoping they would somehow go away. For the first week, my husband’s mother stayed with us. She assisted in watching him at night so that we could get some rest. But I couldn’t sleep. I was devastated, depressed, and terrified. Overwhelmed and crying, I texted my sister, “there is something wrong with me.” She assured me it was normal, and everything settled down after 60 days. But my final text to her that night said, “I don’t think I love him (my son).”

I had no idea what I was up against; no one in my family had ever suffered through postpartum depression. My biggest fear was that I would end up on the news that I would harm or kill my child. During this rough period, I did the only thing I could truly admire about myself…I informed everyone around me that I was “sick.” Many of the responses were that it was normal. I was even told it was a result of my “gut” and deficiencies in vitamins. I felt pressured to breastfeed, although it was one of my biggest triggers aside from my son crying. I felt ashamed to give my son formula by my in-laws. I would hear my mother-in-law arguing with my husband outside our bedroom. I felt so insecure about my underproduction that I would feed my son formula throughout the day and pump breastmilk to the store so she could feed him when she’d watch him. I hid that I couldn’t produce enough or that he wouldn’t latch. I even recall a moment when 2 ounces of breastmilk spilled, and I nearly had a mental breakdown.
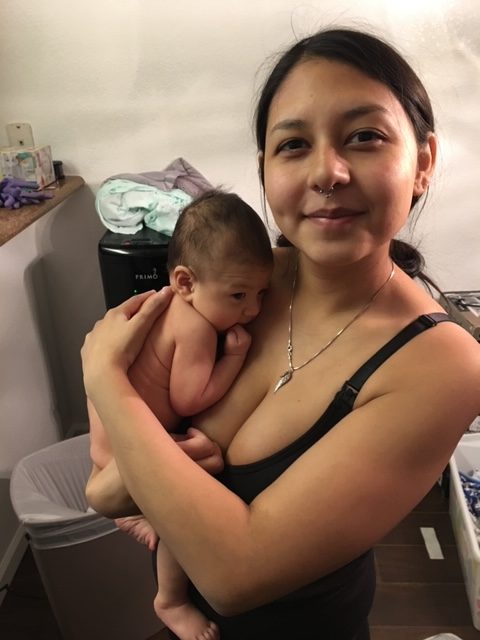
Returning to work was a relief. It allowed me to focus on feeling like an adult again and not feeling “broken” at home. No one at work knew I was suffering, and that helped. Everyone talked about how devastating it was to be away from their newborns, which made me feel guilty. For the next eight months, I didn’t spend longer than a few minutes alone with my son. I stayed at my sister’s after work every day until midnight, when my husband came home. I endured so many moments of pain during this period. My in-laws would often talk about me in reference to mental health, although I sat across the room. Every word pierced me, I had always held myself highly as an intellectual person, and now I felt stripped, insulted, betrayed, and certain they thought I was “crazy”. . Yet, all I could do was thank them for helping me with my son while I was at work.




I recall nights being the most difficult. It was November, so it would become dark around 5 pm and extremely cold. My son slept at 1 ½ to 2-hour intervals. I often questioned how much sleep deprivation it took to die. Due to my stitches, I was scared to eat solids (because stools could tear your stitches), so I often didn’t eat and just consumed coffee as a pick-me-up. I almost felt “fine” in the day (I usually had my family help with my son), but it would fall apart at night. I recall lighting multiple candles and even leaving our Christmas tree up to distract me from the “darkness.”

One memory that stands out to me is when my husband and I were sitting on our couch. My mother-in-law had just put my son to bed and take him to her room. I recall crying, telling my husband I was no longer “me.” How unfair it was that everything I’d ever been proud of, every trait I’d ever developed, was gone, and all I had left were little glimpses of memories. I often had dark thoughts in my head, and sometimes they consisted of fantasizing if I abandoned my family or ended my life or if we lost our son and if our life could get back to “normal.” Every day I felt like I was battling for my soul, and the best I could do some days was ignore my thoughts. I’d block the dark thoughts, pay no attention to them, and mindlessly complete my duties as a mother. I stopped trying to ask myself if things would get better and focused on completing one day at a time.







Many times in my journey, I felt “recovered” and then would relapse. I knew I’d relapse because from feeling secure and understanding my son, I’d suddenly feel terrified and like he was a stranger. His cries would send chills throughout my body, and nothing could keep me warm. I had a breakthrough about 2-3 months postpartum where I recall looking at my husband and telling him, “I think I love him.”
I am 2 years postpartum, and I truly love being a mother. I never knew I could feel so at peace and overwhelming love. Sometimes at work, I almost start crying when I think about how much I miss and love him and watch his videos or look at his pictures on my lunch break. He drives me; he inspires me. I could not, nor do not ever want to picture my life without him. Oliver is my best friend and the little love of my life.





When I watch the news and see stories about mothers who harmed their children, it truly breaks my heart. I don’t know why I was blessed with the ability to recover, but I recall feeling so close to losing the battle. To all those women, I am so sorry they lost the fight. And yes, it is a fight. I remember two different personalities and voices fighting in my head between what was right and how I felt. As mentioned, it didn’t feel only like “depression” I felt like I was splitting into multiple personalities.
What I felt was most essential for my recovery was the love and understanding I had from my family and my husband. My husband allowed me to speak freely regarding all my emotions and thoughts. My family held and loved my son when I couldn’t. I am eternally grateful to them for that.


Signs of postpartum depression and/or anxiety are not limited to but may include:
- Withdrawing from family and friends
- Crying or feeling sad more than you normally do.
- Feeling disconnected from your infant.
- Feelings of anger, confusion, disorientation.
- Feeling guilty or ashamed of not being a good mom.
If you or someone you know may be struggling through postpartum depression or anxiety, please reach out for help. Contact your healthcare provider, and if you are experiencing thoughts of harming yourself or your baby, please call 1-800-273-8255.
[…] types of sessions are a way of me giving back to the community and telling the stories of individuals, families, and causes. I typically shoot two of these a […]